A boil is a common skin problem that often causes concern because of its painful appearance and rapid changes.
Many people notice a tender red bump on their skin and immediately wonder whether it is a pimple, an insect bite, or something more serious.
Understanding what a boil looks like can help you identify it early and know when it may need medical attention.
Boils develop when bacteria infect a hair follicle or oil gland, leading to swelling, redness, and the buildup of pus beneath the skin.
While some boils remain small and heal on their own, others can grow larger, become more painful, and even spread infection if not properly treated.
Their appearance can change significantly over time, which is why recognizing each stage is important.
In this article, we will explain what a boil looks like at every stage, how it feels, where it commonly appears, and when it is time to see a doctor.
What Is a Boil?
A boil, medically known as a furuncle, is a painful skin infection that develops deep inside a hair follicle or oil gland. It occurs when bacteria most commonly Staphylococcus aureus enter the skin through a tiny cut, scrape, ingrown hair, or irritated pore. Once inside, the bacteria trigger the body’s immune response, leading to inflammation, swelling, and the formation of pus.
Boils usually start small but can grow quickly as the infection worsens. Unlike pimples, which affect only the surface of the skin, boils form deeper and are often much more painful. As white blood cells rush to fight the infection, dead tissue and bacteria collect in the center, creating a pus-filled core. This is what gives a boil its characteristic swollen, tender appearance.
Boils can appear anywhere on the body, but they are most common in areas where skin rubs together or where sweating is frequent, such as the face, neck, armpits, thighs, buttocks, and groin. While a single boil may resolve on its own, multiple boils appearing together are known as a carbuncle, which is a more serious condition that may require medical treatment.
Although boils are usually not dangerous, they can become severe if left untreated, especially in people with weakened immune systems. Understanding what a boil is helps distinguish it from other skin conditions and ensures proper care at the right time.
What Causes Boils?
Boils develop when bacteria infect a hair follicle or oil gland beneath the skin. The most common cause is Staphylococcus aureus, a type of bacteria that normally lives on the skin without causing problems. However, when this bacteria enters the skin through a small break such as a cut, scrape, insect bite, or ingrown hair it can trigger an infection that leads to a boil.
Poor skin hygiene can increase the risk, as bacteria are more likely to multiply on unclean skin. Excessive sweating also plays a role by creating a warm, moist environment where bacteria thrive. This is why boils often appear in areas that experience friction and sweat, such as the armpits, groin, thighs, and buttocks. Tight clothing that rubs against the skin can further irritate hair follicles, making infection more likely.
Certain health and lifestyle factors can also make someone more prone to boils. People with weakened immune systems, diabetes, obesity, or chronic skin conditions are at higher risk. Frequent shaving or waxing can cause tiny cuts in the skin, allowing bacteria to enter more easily. In some cases, close contact with someone who has boils or sharing personal items like towels or razors can spread bacteria and lead to infection.
While anyone can develop a boil, repeated or recurrent boils may indicate an underlying issue that needs medical evaluation. Understanding the causes of boils is essential for both effective treatment and prevention, helping reduce the chances of future infections.
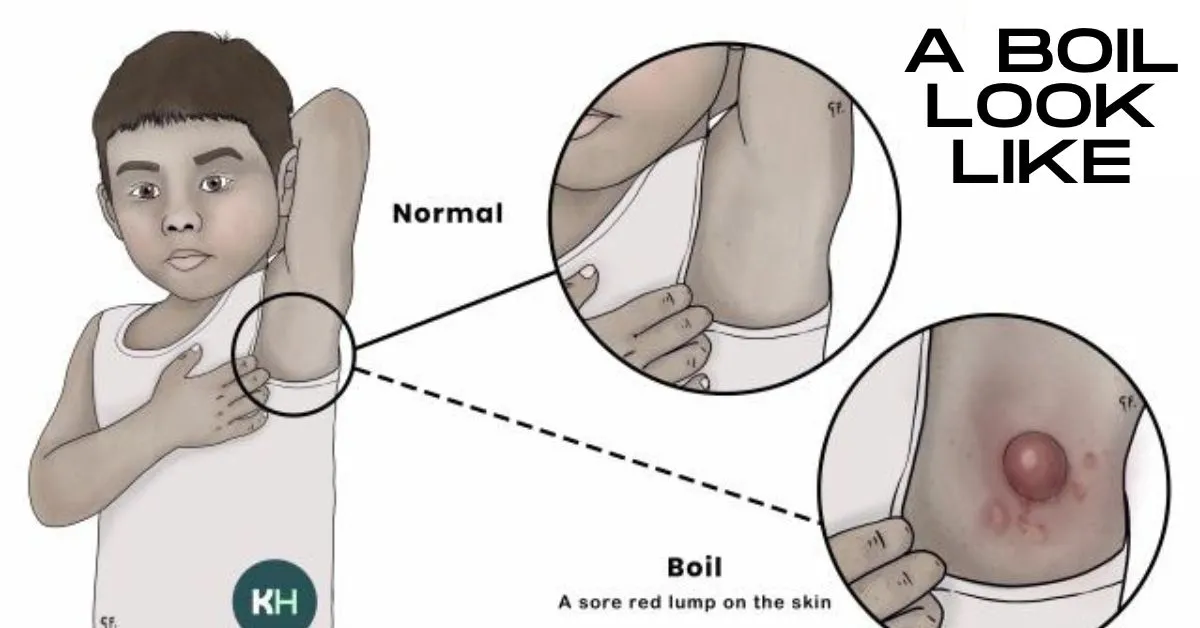
What Does a Boil Look Like?
The appearance of a boil changes as the infection progresses, which can make it confusing to identify at first. In the early stage, a boil usually starts as a small, red, and tender bump on the skin. It may feel firm to the touch and slightly painful, similar to a pimple or an insect bite. At this point, there is minimal swelling, and the area may feel warm but not severe.
As the infection worsens, the boil enters the inflammatory or growing stage. During this phase, the bump becomes larger, more swollen, and increasingly painful. The surrounding skin often turns bright red and may look shiny or stretched. Pressure and throbbing sensations are common, and the boil may feel hard due to inflammation beneath the skin.
In the mature or pus-filled stage, the boil develops a visible yellow or white center. This indicates the buildup of pus, which consists of dead tissue, bacteria, and white blood cells. The boil may feel softer in the middle and extremely tender. Pain is usually at its peak during this stage, and movement or friction can make discomfort worse.
Finally, the boil reaches the draining and healing stage. It may open on its own and release pus, which reduces pressure and pain. A scab forms as the skin heals, and redness gradually fades. Healing can take several days to weeks, sometimes leaving a small scar. Recognizing these stages helps determine whether home care is enough or medical treatment is needed.
What Does a Boil Feel Like?
A boil does not only change in appearance as it develops; the way it feels also shifts noticeably from stage to stage. In the early phase, a boil often feels like a small, sore lump under the skin. It may be mildly painful or tender when touched and can cause slight irritation or itching. At this stage, discomfort is usually manageable and may be ignored or mistaken for a minor skin issue.
As the boil grows, the pain becomes more intense. The affected area often feels warm, tight, and swollen due to inflammation beneath the skin. Pressure builds as pus accumulates in the center, causing throbbing or aching pain. Everyday movements, clothing friction, or even light contact can significantly increase discomfort, especially if the boil is located in a high-friction area like the armpit or inner thigh.
During the mature stage, the boil is typically at its most painful. The skin may feel stretched and sensitive, and the center of the boil can feel soft or “squishy” compared to the firm surrounding tissue. This combination of firmness and softness is a key sign that pus has formed. Some people also experience a pulsating sensation due to increased blood flow to the infected area.
Once the boil drains, pain usually decreases quickly. The area may still feel sore or tender, but the sharp pressure sensation fades. As healing progresses, discomfort gradually subsides, leaving mild sensitivity until the skin fully recovers. Understanding how a boil feels can help you recognize its stage and decide when medical care may be necessary.
What Color Is a Boil?
The color of a boil can provide important clues about its stage and severity. In the early stage, a boil usually appears red or pink due to inflammation. This redness is caused by increased blood flow as the body responds to the bacterial infection. At this point, the skin may look slightly swollen but uniform in color, similar to an irritated bump or inflamed pimple.
As the boil grows and the infection deepens, the redness often becomes darker and more intense. The surrounding skin may appear bright red, deep red, or even purplish, especially if the inflammation is severe. The area can also look shiny or stretched as swelling increases. In people with darker skin tones, a boil may appear deep red, brownish-red, or purple rather than bright red, which is important to recognize to avoid misdiagnosis.
When the boil reaches the pus-filled stage, a yellow or white center usually becomes visible. This color change indicates the buildup of pus beneath the skin, made up of dead tissue, bacteria, and immune cells. The contrast between the red outer area and the pale center is a classic sign of a mature boil.
During the healing stage, the color gradually changes again. After drainage, the area may look less red and begin to form a brown or dark scab. Over time, the skin fades back to its normal tone, though temporary discoloration or a faint scar may remain. Monitoring color changes helps determine whether a boil is healing properly or worsening.
How Big Can a Boil Get?
The size of a boil can vary widely depending on the severity of the infection, its location, and how early it is treated. In the early stage, a boil is usually small, often about the size of a pea or small marble. At this point, it may feel like a firm bump under the skin with mild swelling and tenderness.
As the infection progresses, the boil can grow rapidly. Many boils reach the size of a grape, walnut, or even a golf ball as pus continues to collect in the center. The surrounding skin may swell beyond the visible bump, making the affected area appear larger than the boil itself. Larger boils are typically more painful and may interfere with movement, especially if they develop in areas such as the armpits, groin, thighs, or buttocks.
In some cases, multiple boils can form close together and merge into a carbuncle. Carbuncles are significantly larger than single boils and may involve several infected hair follicles. They often cause more severe pain, swelling, and sometimes fever or fatigue. Because of their size and depth, carbuncles usually require medical treatment.
While small boils often heal on their own, a boil that continues to grow beyond two inches in diameter, becomes extremely painful, or does not improve within one to two weeks should be evaluated by a healthcare provider. Size is an important indicator of severity and can help determine when professional care is necessary.
Common Locations Where Boils Appear
Boils can develop anywhere on the body, but they are most common in areas where hair follicles are abundant, friction occurs, or sweat tends to accumulate. Understanding typical locations helps identify boils early and differentiate them from other skin issues.
The face and neck are frequent sites for boils, particularly around the jawline and hairline. These areas are prone to bacterial entry from shaving, acne, or minor cuts. Facial boils can be more sensitive due to thin skin and may cause swelling that is noticeable and uncomfortable.
Armpits are another common location because sweat, friction, and trapped bacteria create an ideal environment for infection. Boils here can be particularly painful when raising or moving the arms. Similarly, the groin, inner thighs, and buttocks are prone to boils because these areas experience heat, moisture, and friction from clothing or physical activity.
Boils can also appear under the breasts, where sweat and skin folds increase the likelihood of bacterial infection. In men, boils may develop on the chest, back, or shoulders, often associated with sweat or friction from tight clothing.
In some cases, boils appear on hands or fingers, usually near nail beds or cuts, as bacteria can enter through minor wounds. Rarely, boils may form on the scalp, particularly under thick hair, where irritation or poor hygiene provides a breeding ground for infection.
Knowing these common locations helps in early recognition, proper hygiene, and prompt treatment. Boils in sensitive areas like the face, groin, or spine may require medical attention sooner, while those in less sensitive areas can often be managed at home.
Types of Boils
Boils can vary in size, severity, and location, and understanding the different types can help determine the best approach for treatment. The most common type is a single boil, or furuncle, which develops in a single hair follicle. It usually starts as a red, tender bump and can grow to become pus-filled over time. Single boils are the most common form and often heal on their own with proper home care.
When multiple boils appear close together, they may merge to form a carbuncle. Carbuncles are larger, deeper infections that involve several hair follicles. They are typically more painful than single boils and can cause systemic symptoms such as fever, fatigue, or swollen lymph nodes. Carbuncles often require medical treatment, including drainage and sometimes antibiotics.
Some boils are cystic, meaning they form deeper under the skin and may feel firm and round. These boils may persist longer than typical furuncles and can leave a scar if not treated carefully. Recurrent boils are another type, where an individual experiences repeated outbreaks over weeks or months. Recurrent boils may indicate an underlying health issue, such as diabetes, weakened immunity, or chronic skin irritation.
Boils can also be classified by location. For example, facial boils are often more sensitive and require extra caution, while armpit or groin boils are associated with friction and sweating. Understanding the type of boil is essential for proper care. While many boils heal at home, certain types like carbuncles or recurrent boils may require medical attention to prevent complications.
Boil vs Other Skin Conditions (Visual Comparison Guide)
Not every red bump on the skin is a boil. Understanding the differences between boils and similar skin conditions helps prevent misdiagnosis and ensures proper treatment.
A pimple, for instance, is usually smaller and less painful than a boil. Pimples form on the skin’s surface and often contain a small amount of pus. In contrast, a boil develops deeper under the skin, is larger, and tends to be more tender and swollen. Pimples usually heal faster and rarely require medical intervention, while boils can persist for days or weeks.
A cyst is another condition that can resemble a boil. Cysts are usually firm, round lumps beneath the skin and may not be red or painful unless infected. Unlike boils, cysts are often chronic and can remain for months without changing in size. Surgical removal may be necessary for cysts, whereas most boils resolve naturally or with minor medical care.
An abscess is a collection of pus that can appear similar to a boil, but abscesses are generally larger, more painful, and often accompanied by fever or general malaise. Abscesses almost always require professional drainage and antibiotics.
Ingrown hairs can also mimic boils, especially in areas where shaving occurs. They appear as small, red, and sometimes pus-filled bumps. The key difference is that an ingrown hair usually has a visible hair trapped beneath the skin, whereas a boil forms around an infected follicle with pus accumulation.
Lastly, spider bites or minor skin infections can sometimes look like boils but usually heal faster and are less painful. Recognizing these distinctions helps ensure proper treatment and reduces the risk of complications.
Say “next” when you’re ready to continue to the next section.
next and 250 words count
Are Boils Contagious?
Boils are primarily caused by bacteria, most commonly Staphylococcus aureus, which can live on the skin without causing harm. While the bacteria themselves are contagious, the boil itself is not directly “catchable” like a cold. However, under certain conditions, boils can spread from person to person or from one area of the body to another.
Direct skin-to-skin contact with an infected area is one of the main ways boils can spread. Touching the pus, drainage, or the surface of an open boil can transfer bacteria to another person or another part of your own body. Sharing personal items, such as towels, razors, clothing, or bedding, can also allow bacteria to spread, increasing the risk of new boils forming.
Good hygiene practices are essential to prevent transmission. Always wash hands thoroughly after touching a boil, and avoid sharing personal items. Covering a draining boil with a clean bandage reduces the chance of spreading bacteria. People with weakened immune systems, diabetes, or other underlying health conditions are at a higher risk of developing boils from exposure to bacteria.
Although most boils are not highly contagious, it’s important to monitor skin carefully and take precautions until the infection has fully healed. Recurrent boils in a household may indicate the need for extra hygiene measures, including disinfecting commonly touched surfaces and laundering clothing or towels frequently.
By understanding how boils spread, you can take steps to protect yourself and others while allowing the infection to heal safely.
Should You Pop a Boil?
It can be tempting to squeeze or pop a boil to relieve pressure or speed up healing, but doing so is strongly discouraged. Popping a boil at home can push bacteria deeper into the skin, increasing the risk of a more serious infection or creating a larger abscess. It can also lead to scarring or permanent skin damage.
Boils contain pus, which is made up of dead tissue, bacteria, and white blood cells. While it may look tempting to release this fluid, the body often drains the boil naturally when it reaches the right stage. Interfering prematurely can slow healing and spread bacteria to nearby skin or even other people.
Using unclean tools or fingers to pop a boil significantly raises the chance of secondary infections. In some cases, improper popping can lead to bloodstream infections or cellulitis, a dangerous skin infection that requires immediate medical attention. Even after drainage, the skin may remain tender and prone to further infection if not cared for properly.
The safest approach is to allow a boil to mature naturally while keeping it clean and covered with a sterile bandage. Applying warm compresses can help encourage natural drainage, reduce pain, and speed up healing. If a boil becomes extremely large, very painful, or fails to drain on its own, a healthcare provider may perform a professional incision and drainage procedure in sterile conditions.
Understanding why popping a boil is risky helps prevent complications, protect the surrounding skin, and ensure proper healing without leaving lasting scars.
How to Treat a Boil at Home
Most small boils can be treated safely at home with simple care measures, especially in the early stages. The primary goal is to encourage natural drainage, reduce pain, and prevent infection from spreading.
One of the most effective home treatments is applying a warm compress to the affected area. Soak a clean cloth in warm water and place it on the boil for 10–15 minutes, several times a day. The heat helps increase blood circulation, which allows white blood cells to fight the infection and encourages the pus to come to the surface.
Keeping the area clean is essential. Wash your hands before and after touching the boil, and gently clean the skin around it with mild soap and water. Cover the boil with a sterile bandage to protect it from friction and contamination. Change the bandage whenever it becomes wet or dirty.
Avoid squeezing or popping the boil, as this can push bacteria deeper into the skin, causing more serious infection or scarring. Over-the-counter pain relievers like acetaminophen or ibuprofen can help reduce pain and inflammation.
Hydration, rest, and a healthy diet also support the body’s immune system, helping it fight the infection more efficiently. In most cases, a small boil will drain naturally and heal within one to two weeks with these measures.
However, if the boil becomes larger, extremely painful, shows signs of spreading infection (red streaks, fever), or does not improve after a few days of home care, it is important to seek medical attention. Proper home care combined with medical guidance when needed can prevent complications and promote faster healing.
Medical Treatment for Boils
While many boils heal with home care, some require professional medical treatment, especially when they are large, recurrent, or complicated. Medical intervention is necessary when a boil does not improve, causes severe pain, spreads infection, or forms a carbuncle.
One of the most common medical procedures is incision and drainage (I&D). In this procedure, a healthcare provider numbs the area and makes a small cut to drain the pus safely. This reduces pressure, relieves pain, and allows the infection to heal more quickly. Attempting this at home is strongly discouraged because it can worsen the infection, cause scarring, or spread bacteria.
In addition to drainage, antibiotics may be prescribed if the infection is severe, spreading, or associated with fever. Oral antibiotics help fight the bacterial infection from within, while topical antibiotics may be applied to reduce local bacterial growth. Patients with recurrent boils or underlying conditions, such as diabetes or immune deficiencies, may also undergo further tests to identify predisposing factors.
For carbuncles or boils located on the face, spine, or other sensitive areas, medical attention is especially important due to the risk of serious complications, including the spread of infection to deeper tissues or the bloodstream.
Even after medical treatment, proper wound care is crucial. The area should be kept clean and covered, and follow-up visits may be recommended to ensure complete healing. Early medical intervention for complicated boils helps prevent complications, speeds up recovery, and reduces the risk of scarring or further infections.
Say “next” when you’re ready to continue to the next section.
next and 250 words count
Signs a Boil Is Serious or Infected
While most boils are minor and heal with proper care, some indicate a more serious infection that requires medical attention. Recognizing the warning signs of a severe boil can prevent complications and ensure timely treatment.
One of the most common signs of a serious boil is rapid growth. If the boil enlarges quickly over a few days, it may indicate that the infection is spreading deeper into the skin. Severe pain and tenderness, especially if it worsens rather than improves, is another warning sign. Boils that feel extremely firm or pulsating may also suggest an accumulation of pus that needs professional drainage.
Red streaks radiating from the boil toward the heart can indicate that the infection is spreading through the lymphatic system, which is a medical emergency. Similarly, fever, chills, or fatigue accompanying a boil suggest a systemic infection that may require antibiotics or hospital care.
Boils located on sensitive areas, such as the face, spine, or groin, are more prone to complications. Facial boils, for example, can potentially spread infection to the brain if left untreated. Multiple boils appearing simultaneously, or recurrent boils in the same area, may signal an underlying health issue, such as diabetes or a weakened immune system, and should be evaluated by a healthcare provider.
If any of these signs are present, it is important not to attempt home drainage. Instead, seek medical attention promptly. Early intervention can prevent severe infections, reduce pain, and minimize the risk of scarring or more serious health complications.
How Long Do Boils Last?
The duration of a boil varies depending on its size, location, severity, and whether it receives proper care. Most small, uncomplicated boils will go through their natural stages formation, maturation, drainage, and healing within one to two weeks. During this time, the boil may feel increasingly painful as it fills with pus, then gradually soften as it drains naturally.
Larger boils or those located in areas prone to friction, such as the armpits, groin, or buttocks, may take longer to heal, sometimes two to three weeks. Pain often peaks before drainage occurs and usually subsides once pus is released. Proper home care, including warm compresses and keeping the area clean, can help speed up healing and reduce discomfort.
Carbuncles, which are clusters of boils, generally last longer than single boils. They may persist for several weeks and often require medical intervention, including incision and drainage or antibiotics. Recurrent boils may also take longer to resolve and may indicate an underlying health condition that needs attention.
Factors that influence healing time include overall health, immune system strength, hygiene, and whether the boil becomes infected further. People with diabetes, weakened immunity, or chronic skin conditions may experience slower healing and are more prone to complications.
Although small boils usually resolve without medical treatment, persistent, unusually large, or painful boils that do not improve after a week or two should be evaluated by a healthcare provider. Timely care ensures faster recovery, reduces the risk of spreading infection, and helps prevent scarring.
Say “next” when you’re ready to continue to the next section.
next and 250 words count
Scarring After a Boil
Scarring is a common concern for many people after a boil has healed. The risk of scarring depends on the size and depth of the boil, the stage at which it was treated, and individual skin type. Small boils that heal naturally or with proper care often leave minimal or no visible marks, while larger or deeper boils, especially those that required drainage, may leave a temporary or permanent scar.
A boil can damage the skin’s underlying tissue as it fills with pus and stretches the surrounding area. Once the boil drains and the skin begins to heal, a raised or discolored mark may form. Initially, scars may appear red or purple but typically fade over time to a lighter shade. In some cases, scars may become hypertrophic (raised) or keloid (thick and firm), particularly in individuals prone to keloid formation.
Preventing scarring involves careful management during the healing process. Avoid picking at or squeezing the boil, as this can worsen tissue damage. Keep the area clean, apply a gentle antiseptic or antibiotic ointment if recommended, and protect the skin from friction or trauma. Moisturizers or silicone-based gels can also support healing and reduce scar formation.
For persistent or severe scarring, dermatological treatments such as laser therapy, chemical peels, or microneedling may help improve skin appearance. Consulting a dermatologist is especially important for facial boils, where scarring may be more noticeable.
Understanding how boils affect the skin and taking proper care during healing can significantly reduce the likelihood of scarring and support smoother, healthier skin.
How to Prevent Boils
Preventing boils is often possible with good hygiene, lifestyle adjustments, and attention to skin health. Since boils are caused by bacteria entering the skin through hair follicles or small cuts, keeping the skin clean and protected is the first step in prevention. Daily washing with mild soap and water helps remove excess bacteria and reduces the risk of infection.
Avoid sharing personal items such as towels, razors, or clothing, as these can transfer bacteria between people. People prone to boils should also disinfect frequently touched surfaces and launder bedding and clothing regularly. Wearing loose-fitting clothing made of breathable fabrics reduces friction and sweating, which are common triggers for boils in areas like the armpits, groin, and thighs.
Proper shaving techniques can also help prevent boils. Shaving in the direction of hair growth, using clean razors, and moisturizing the skin afterward reduces irritation and the risk of ingrown hairs, which can become infected. For individuals who sweat heavily, keeping the skin dry and changing out of damp clothing promptly can further reduce the risk.
Boosting overall immune health is another preventive measure. Eating a balanced diet, staying hydrated, managing stress, and getting adequate sleep strengthens the body’s natural defenses against bacterial infections.
People with chronic health conditions, such as diabetes or weakened immunity, should monitor their skin carefully and work with a healthcare provider to manage risk factors. By combining hygiene, clothing choices, and lifestyle habits, many boils can be prevented, reducing pain, scarring, and the need for medical treatment.
Boils in Special Situations
While boils can affect anyone, certain situations or health conditions make them more frequent, severe, or complicated. Understanding these special scenarios helps in managing boils safely and preventing complications.
Boils during pregnancy may occur due to hormonal changes and a temporarily altered immune response. Pregnant individuals should avoid self-draining boils and consult a healthcare provider before using any medication, including antibiotics or topical ointments, to ensure safety for both mother and baby.
Boils in people with diabetes are more common and tend to heal slower. High blood sugar levels can impair the immune system, making it easier for bacteria to infect hair follicles. Prompt medical attention is important in these cases, as infections can progress quickly and increase the risk of complications.
Boils in children are usually small and can often be managed at home with warm compresses and hygiene measures. However, children are more likely to scratch or touch boils, which increases the risk of spreading bacteria. Parents should monitor children closely and consult a doctor if boils persist or multiply.
Recurrent boils those that appear repeatedly in the same person may indicate an underlying issue such as a weakened immune system, chronic skin irritation, or a persistent bacterial carrier state. Medical evaluation is essential for recurrent boils to identify the cause and prevent future infections.
Boils in special situations require extra care and vigilance. Avoiding home drainage, maintaining strict hygiene, and seeking timely medical attention can reduce the risk of severe infection, scarring, or systemic complications, ensuring safe recovery.
Say “next” when you want to continue to the next section.
next and 250 words count
Frequently Asked Questions (FAQ) About Boils
Boils are common, and people often have questions about their causes, symptoms, and treatment. Answering these frequently asked questions helps clarify concerns and guides proper care.
Do boils go away on their own?
Small, uncomplicated boils often resolve naturally within one to two weeks. Applying warm compresses and keeping the area clean usually helps the boil mature, drain, and heal without medical intervention.
How do you know if a boil is healing?
A healing boil typically softens, drains pus naturally, and shows reduced redness and pain. The surrounding skin may remain slightly tender, but swelling and throbbing gradually decrease. Scab formation usually follows drainage.
Can boils come back?
Yes, some people experience recurrent boils, especially if they carry Staphylococcus aureus bacteria, have chronic skin irritation, or underlying conditions like diabetes or a weakened immune system. Recurrent boils may require medical evaluation.
Are boils dangerous?
Most boils are not serious and heal with proper care. However, large boils, carbuncles, boils on the face or spine, or those accompanied by fever, red streaks, or swelling can indicate a severe infection and require medical attention.
Can stress cause boils?
Stress indirectly contributes to boils by weakening the immune system, making the body more susceptible to bacterial infections. Proper rest, nutrition, and stress management can support skin health and reduce risk.
These FAQs address common concerns and guide readers on when to manage boils at home versus when to seek professional care. Understanding these aspects ensures safe treatment, prevents complications, and promotes faster healing.
Say “next” when you’re ready to continue to the next section.
next and 250 words count
When to See a Doctor
While many boils heal naturally with home care, there are situations where medical attention is necessary. Recognizing these signs ensures that complications are avoided and treatment is effective.
One clear indicator is a boil that does not improve after one to two weeks of proper home care. Persistent boils may require professional drainage or antibiotics to prevent the infection from worsening. Boils that grow rapidly or become extremely painful also warrant a doctor’s evaluation, as they may indicate a deeper or spreading infection.
Multiple boils appearing at once or a carbuncle are another reason to seek care. Carbuncles involve clusters of boils that merge under the skin and can lead to fever, fatigue, and systemic infection if left untreated. Similarly, boils located in sensitive areas, such as the face, spine, or groin, require medical oversight to prevent complications like scarring or infection spreading to deeper tissues.
Signs of systemic infection, including fever, chills, red streaks radiating from the boil, or swollen lymph nodes, are urgent red flags. These symptoms suggest that bacteria may be spreading through the bloodstream or lymphatic system and need immediate attention.
Individuals with weakened immune systems, diabetes, or chronic skin conditions should be proactive about seeking medical care, even for small boils, as their bodies are more vulnerable to complications.
Visiting a doctor ensures that the boil is drained safely, infection is treated appropriately, and any underlying issues are addressed. Early intervention reduces pain, promotes faster healing, and minimizes the risk of scarring or severe complications.
Say “next” when you’re ready to continue to the final section.
next and 250 words count
Conclusion
Boils are common skin infections that can cause discomfort, pain, and concern. They form when bacteria enter a hair follicle or oil gland, leading to redness, swelling, and pus accumulation.
Understanding what a boil looks like at each stage early, growing, pus-filled, draining, and healing helps in recognizing the condition and deciding whether home care or medical attention is needed.
Most small boils can be managed at home with warm compresses, proper hygiene, and pain relief. Avoiding squeezing or popping the boil is crucial to prevent spreading infection, worsening symptoms, or scarring.
Larger boils, carbuncles, recurrent boils, or boils in sensitive areas require professional care, including drainage and sometimes antibiotics, to ensure safe healing.
Awareness of the warning signs such as rapid growth, severe pain, red streaks, fever, or persistent boils is essential to prevent serious complications.
Individuals with chronic health conditions, weakened immunity, or diabetes should monitor their skin closely and seek medical advice promptly if a boil develops.
Preventive measures, including maintaining cleanliness, managing sweat, using proper shaving techniques, wearing breathable clothing, and supporting overall immune health, can reduce the likelihood of developing boils.
In summary, recognizing the appearance, feel, and progression of boils empowers individuals to respond appropriately, manage discomfort effectively, and protect their skin.
By combining attentive care, hygiene, and timely medical intervention when necessary, most boils heal safely and with minimal lasting effects. Proper understanding and early action are key to ensuring a smooth recovery and preventing recurrence.

Amina Khalid is a registered clinical psychologist and certified Behaviour Support Practitioner based in Brisbane, Australia. With a Doctorate in Clinical Psychology and more than a decade of experience supporting families, caregivers, and individuals with complex behavioural needs, she is known for her compassionate approach and evidence‑based practice. Amina also lectures in clinical and counselling psychology and specializes in psychometric assessment and capacity‑building interventions for children and adults.